Do Weight Loss Medications Like Wegovytm Benefit Afib Patients?
If you follow the news and social media, you’ve undoubtedly seen the meteoric rise in (and shortage of) GLP-1 agonist medications, usually administered via injection into the stomach, like WegovyTM. This medication, also known as Semaglutide, has shown exceptional weight loss potential by targeting certain metabolic functions, leading to less hunger and consequent weight loss. Semaglutides’ rise started as a treatment for Type-2 diabetes known as OzempicTM. Not only was it very effective in this capacity, but significant weight loss was seen in patients taking the drug. Wegovy, a higher-dose version of Ozempic, was approved by the FDA last year for weight loss.
Having researched atrial fibrillation, and its causes, you may know that a significant risk factor for de novo or worsened Afib and cardiac arrhythmias, in general, revolves around lifestyle, specifically diet. As the quality of our collective diets has progressively declined, with more and more Americans classified as overweight and obese, the incidence of heart palpitations and other metabolic diseases like type-2 diabetes, high cholesterol, and high blood pressure have all proliferated.
Next Steps After a Hospital Diagnosis of Afib

Atrial fibrillation, or afib, is common, with approximately 5 million Americans suffering from the condition and a general upward trend in new diagnoses. The causes of Afib and other arrhythmias are many and varied. But age and lifestyle factors are two primary reasons this condition is growing in prevalence here and around the world. Yet, despite this, it is misunderstood for several reasons.
What Your Waist Size Says About Your Heart Health

When we talk about excess weight, and in particular obesity, the body mass index or BMI is almost universally used. The BMI offers an easy way to calculate whether you are considered underweight, normal, overweight, or obese. Using these classifications, we can get a pretty good idea of who is at risk of the disease associated with morbid obesity, including cardiovascular disease. However, these BMI thresholds and classifications are ultimately arbitrary; in other words, not all patients with the same BMI will have the same risks or symptoms.
As a result, there is ongoing research into refining the BMI into a tool that can better approximate the risk of disease associated with excess weight. Until that is achieved, waist size and waist-to-hip ratio (a measure of where patients hold their extra body fat) can be a far better predictor of heart disease than BMI. Men with a waist size of 40 or more and women with a waste of 35 or more have been correlated with a significantly higher risk of heart disease, and this correlation is somewhat independent of BMI.¹
Dr. Moretta’s Left Bundle Branch Pacing Presentation at Sarasota Memorial Hospital
Dr. Moretta’s Presentation on LBB Pacing
Click on the link above to view Dr. Moretta’s Left Bundle Branch Pacing Presentation at Sarasota Memorial Hospital.
Announcing Dr. Moretta’s Participation in Conduction System Pacing Study
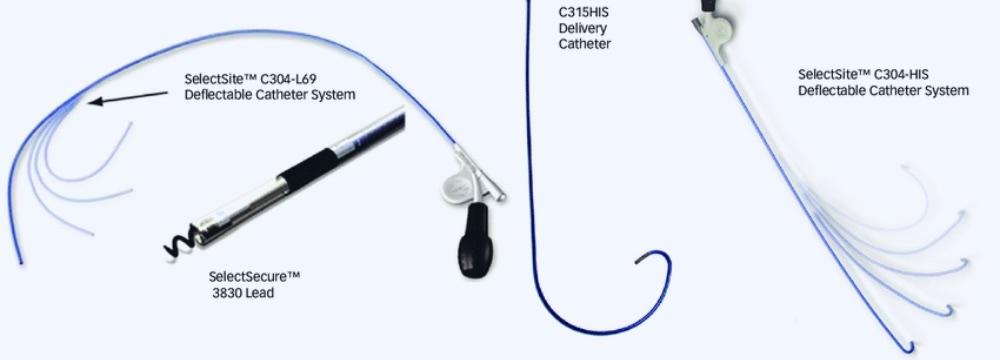
In the spirit of bringing to you the latest news in electrophysiology and our practice, Dr. Moretta is thrilled to have been chosen as a study center for the BIOTRONIK Conduction System Pacing with the Solia Lead clinical trial. Our program was the third facility, after NYU and Cornell University, to be asked to participate in this trial.
As you may know, Dr. Moretta is a proponent of conduction system pacing and a leader in its adoption. It offers potentially significant benefits over traditional pacemakers, and this study will help solidify research into those advantages. Left Bundle Branch (LBB) pacing is a particularly exciting research focus in this area.
Dementia Risk in Afib Patients Treated With Catheter Ablation vs. Antiarrhythmics
The treatment for atrial fibrillation, or Afib, runs on a continuum of care that begins with the least invasive options and typically ends with a minimally invasive cardiac catheter ablation to destroy problematic heart tissue causing the arrhythmia permanently. When we started treating Afib with procedural options, we often prioritized other methods of care simply because, at the time, we did not have the precision and technological advancement that we enjoy today. However, as technology and technique have improved, cardiac catheter ablation has become an ever-more viable early-stage intervention. It can, in qualifying patients, be successful 70 or even 80% of the time.
With that said, whether medication therapy should be started or continued or whether a potentially curative procedural solution should be undertaken is a conversation that each patient will have with their electrophysiologist. However, recent data has given us additional insight into whether antiarrhythmic medication or procedure cardiac catheter ablation is preferable regarding dementia risk in Afib patients.
Silent Afib – A Non-Issue or Something to Be Concerned About?
When we discuss arrhythmias, and in particular, the most common arrhythmia, atrial fibrillation (Afib), we usually think about it in the context of significant and sometimes debilitating symptoms that can include a rapid heartbeat, the sensation of the heart beating out of the chest, sweating, fainting, nausea, and breathlessness. These are all hallmark symptoms of this most prevalent heart rhythm disorder. Typically, patients are well aware of these heart rhythm irregularities and seek care from their primary care physician or cardiologist. Some even end up in the emergency room, thinking they have experienced a heart attack. Often, if these paroxysmal or occasional Afib episodes remain untreated, it’s because when they visit their non-arrhythmia specialist, they are hooked up to an EKG, which cannot diagnose an arrhythmia unless they are in active Afib.
However, some patients are diagnosed with an asymptomatic form of Afib known as silent atrial fibrillation. Patients may not have a rapid heartbeat and don’t feel any symptoms. Typically, they are diagnosed with silent Afib during a routine visit to their primary care physician, including an EKG, or it is found incidentally, secondary to another diagnostic test for a different concern or condition.
Dual Procedures for the Management of Afib and Its Stroke Risk
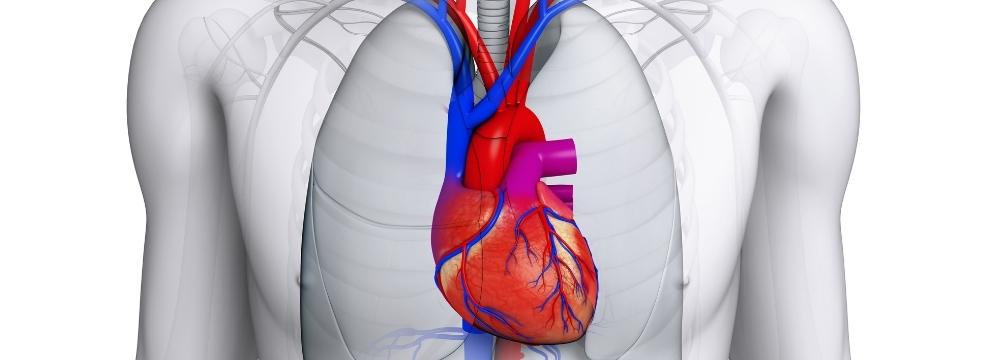
Afib, or atrial fibrillation, is the most common cardiac arrhythmia in the US, with upwards of five million people suffering from the condition. While it may seem innocuous to someone who hasn’t experienced it, significant concerns are associated with Afib beyond the obvious lifestyle impediments and discomfort of a fast-beating heart. The main concern for an electrophysiologist like Dr. Moretta is the significantly increased risk of stroke and heart attack and the longer-term risk of congestive heart failure.
To understand this risk and how a procedural option can make a difference, we must explore the heart and how it works. The heart is divided into four separate chambers. Two upper chambers are known as the atria, and two lower chambers are known as the ventricles; these chambers work in a coordinated manner to receive electrical signals that initiate and coordinate a heartbeat. When these electrical signals begin to malfunction, patients develop an arrhythmia.
Study Shows a Potential Link Between Electronic Games and Dangerous, Even Deadly, Arrhythmias.

We’ve come across a study published this month that discusses an as-of-yet unstudied phenomenon of the potential for dangerous or even deadly arrhythmias in young people associated with electronic games. We’ve previously known that young athletes with congenital heart disorders are at greater risk for arrhythmia during intense physical exertion. This is not surprising as exercise can increase the heart rate dramatically. However, the bigger surprise was that sedentary electronic gaming could also trigger these dangerous arrhythmias leading to unexplained syncope – fainting – and even death in some kids. It’s not hard to understand why this could be the case. Certain games, primarily the very popular first-person, war, adventure, and shooter games, can raise the heart rate dramatically.
Spotlight on Heart Mapping Technology in Electrophysiology
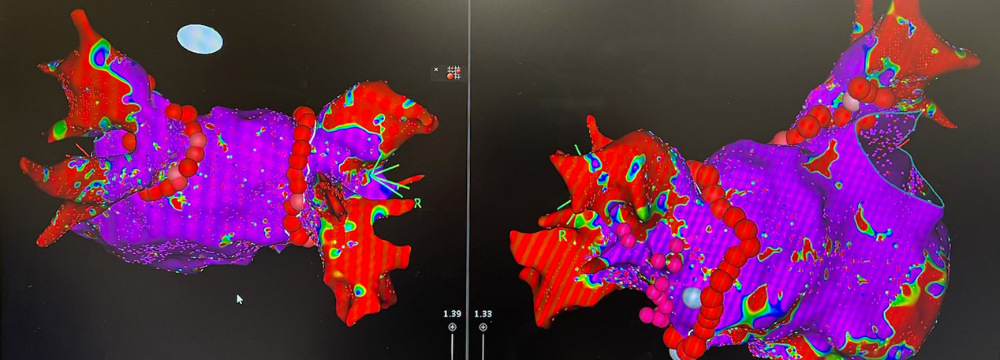
You may remember a prior post on our website discussing the incredible technology we, as electrophysiologists, have at our fingertips. This technology has made treating cardiac arrhythmias, particularly Atrial Fibrillation or Afib, safer and more effective than ever. Another significant benefit of this technology is the time it takes for Dr. Moretta to complete an ablation. What once routinely took 2, 3, 4, or more hours can now be performed in less than an hour and often in as little as 45 minutes. One of the key technological features of any advanced electrophysiology lab is the three-dimensional mapping we use to visualize the structures of the heart and the path and amplitude of the electrical signals that may be causing the arrhythmia. To illustrate this, please have a look at the image below. This is an actual map of the heart of one of our patients enrolled in the REAL-AF study, for which we are a study center. He was the 100th patient we treated for this trial.
